Harvard Men’s Health Watch Published: December, 2018
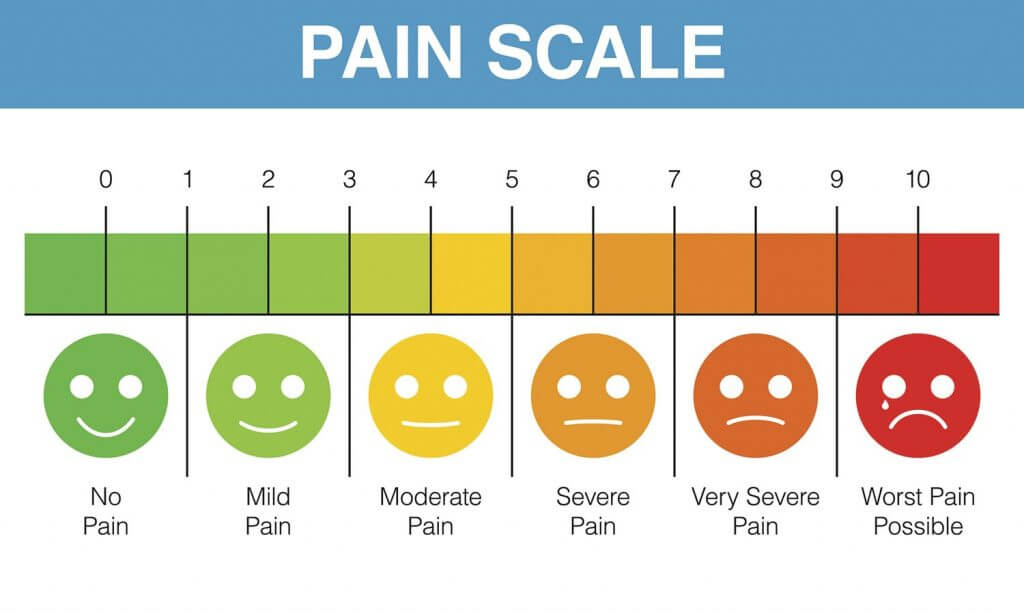
Doctors and patients use the 10-point pain scale to gauge the severity of pain, but there may be a better way.
You may remember being asked to describe your level of pain on a 10-point scale, with 0 meaning no pain and 10 meaning extreme pain.
This scale was initially designed to help nurses and doctors better document and monitor how much pain you were experiencing and thereby offer the right treatment.
“However, we now realize the scale is too simple to measure something so complex,” says Dr. Jianren Mao, chief of the Division of Pain Medicine at Harvard-affiliated Massachusetts General Hospital. “People have a difficult time articulating their pain with just numbers and thus are more likely to be misdiagnosed.”
By the numbers
The 10-point scale was developed in the 1970s as a way for researchers to measure and trace the progress and improvement of pain in studies.
The scale uses either numbers or sketches of facial expressions that correlate with pain levels, like happy, neutral, and sad faces.
It seemed like an easy way for scientists to speak the same language. If a medication lowered the pain ranking from an 8 to a 4 among people who took it, researchers could theorize that the drug might help to reduce pain levels. “Yet, one of the main problems with this approach is that the scale is very individualized,” says Dr. Mao. “What one person rates as an 8 or 4 may be quite different for someone else, so it is not always an accurate assessment.”
A new direction
Researchers have begun to revisit how the pain scale is used. A better approach suggests that the 10-point scale is one way — but not the only one — to measure pain. “Instead of relying on a single number for diagnosis, measuring pain should use a multi-tier approach,” says Dr. Mao. For example:
- Rank the pain. Patients might choose from several categories, like mild, moderate, and severe, with some levels of degree under each one.
- Detail the pain. Provide specific details about where and when the pain occurs, and what makes it better or worse.
- Note frequency and duration. When do flare ups most often strike? Does the pain come and go, or last for a certain amount of time? Do the symptoms fluctuate? When does this occur?
- Describe the pain. Is it dull, sharp, burning, nagging, throbbing?
Look at quality of life
Finally, you and your doctor need to consider how the pain affects your quality of life. “Pain does not always interfere with how you live, no matter what the number,” says Dr. Mao. “If it doesn’t cause any major lifestyle issues, you might be better off taking a wait-and-see approach, or trying another type of therapy before going straight to drug treatment.”
This new approach to measuring pain may sound more complex than the 10-point scale, but the idea is to provide as much detail as possible to your doctor in order to paint the clearest possible picture of your situation. “Only then can you get the specific treatment you need to address your pain, and yours alone,” says Dr. Mao.
